Blog
Time with Swans doc spurring Indigenous student on
Hamish Albany hopes to combine his passion for Indigenous health with his zeal for sports medicine – and his hunger to achieve his dreams is being fuelled by a Sydney Swans apprenticeship.
By Zachary Gates

Hamish Albany hopes to combine his passion for Indigenous health with his zeal for sports medicine – and his hunger to achieve his dreams is being fuelled by a Sydney Swans apprenticeship.
The 23-year-old Indigenous man is getting a real-life taste of the sports-medicine industry in a four-week stint with head Swans doctor Tom Cross, which counts as an elective placement for the Bachelor of Medical Studies/Doctor of Medicine degree he’s tackling at UNSW.
In his four weeks with Dr Cross, Albany is assessing players' injuries, liaising with the physiotherapy team and analysing case studies of past and present Swans who've undergone surgery for piriformis syndrome, a condition in which the piriformis muscle, located in the buttock region, spasms and causes pain.
As the final five days of his four-week stint with Dr Cross tick by, Albany is rapt to have discovered he'd thoroughly enjoy a career in sports medicine.
"It's a bit tricky but in a good way. I just finished an elective where I was doing GP work for a remote Indigenous community, which I absolutely loved. And now in coming to the Swans and doing sports medicine I'm finding this is another field that I'm really passionate about. This elective has definitely given me a lot to think about," Albany said.
"My dream is to work in a remote Indigenous community, but sports medicine is something I'm also really passionate about, so whether I can balance the two I guess we'll see.
"Tom does such a great job as a doctor here at the club and he's really inspired me to become the best doctor I can be. I see him as someone to aspire to be like, and even if I don't end up in the field of sports medicine, he's the type of doctor I want to be."
Albany linked with Dr Cross through the GO Foundation, an organisation co-founded in 2009 by Swans greats Adam Goodes and Michael O'Loughlin, which provides Indigenous students from kindergarten through to university with fully funded scholarships.
Albany, who's now in his sixth and final year of his university degree, doesn't actually have a GO Foundation scholarship, but the impact of the organisation on his life has been enormous nonetheless.
GO Foundation CEO Shirley Chowdhary was a source of guidance as the St Gregory's College graduate struggled in the third year of his university degree, and he now regularly attends GO Foundation events and is a mentor to a host of scholarship-holders.
"GO has been huge for me," Albany said.
"My younger brother Noah, who's in his fourth year of a Bachelor of Law at UNSW, was actually one of the earliest students to graduate with the GO Foundation – and I had an informal introduction to GO through him. I met Goodesy and Micky O' and they've been great mentors for myself and my brother. Shirley, the CEO of GO, has also helped guide me through uni and given me a lot of good advice on how to deal with some of the challenges I've had to face."
In the 10 years since the GO Foundation was established, it has fully funded 210 Indigenous students across 28 schools, four universities and two states.
GO has always supported NSW students since its 2009 inception, and in February 2019 it launched in South Australia, the home state of Goodes and O'Loughlin.
Albany hails from Queensland's Kalkadoon tribe but grew up on Dharawal land, in Campbelltown in Sydney's south-west, after his nan moved to the harbour city.
And while he only ever played rugby league and rugby union as a kid, he said he always idolised Goodes and O'Loughlin on the TV and sees them as role models today.
"It's unreal to know Mick and Adam," Albany said.
"Seeing them play on the TV when I was growing up was amazing, and they've always been big inspirations of mine. They're obviously big sporting heroes but they're also really big with the cultural leadership that they've shown for Indigenous people in Australia. I don't think there'd be many Indigenous people who wouldn't see Mick and Adam as heroes.
"So meeting them at first was quite surreal but I've since found they're actually such genuine people, and they've played a mentoring role for me. It's a funny feeling when you meet someone who you've always looked up to and realise that they're actually just another human.
"It makes you realise that you can shoot for the stars as well."
Winner of The Joe French Award goes to: Dr Sharron Flahive
The John Eales Medal Rugby Australia awards were held late 2019. This wasn't just any awards night, Dr Sharron Flahive was awarded the Joe French Award for her outstanding contribution to Rugby over the last 20 years.
The Stadium clinic is beyond proud of Dr Flahive and her achievements to Rugby, after serving an amazing 20 years at the NSW Waratahs Sharron retired earlier this year and has moved on to be Chief Medical Officer for The Wallaroo's.
She has also been appointed to the Board of the International Rugby Players Association.
Dr Flahive is excited to continue her interest in Player Welfare at an International level, an area that she has always been very passionate about and we are very excited to follow Sharron on her ongoing journey in rugby.
Click here to view video of Joe French Award - Sharron Flahive interview
Click here to view video of Joe French Award - Sharron Flahive interview

8 Tips for Healthy Sleeping
- Don’t drink any fluids 2 hours before bed to prevent night time waking.
- Avoid blue light exposure from computers and phones late in the evening. No TV before bed.
- Put your work away at least an hour before bed to clear the mind. Take a bath, mediate or do some light reading.
- If your mind is racing try writing what’s on your mind down and letting it go until the morning.
- Allow enough time for sleep. 8 hours is ideal for most people.
- Avoid nicotine and caffeine as these are stimulants.
- Exercise during the day.
- Sleep in complete darkness…you could wear an eye mask.
Some herbal medicines and nutrients can also promote restful and restorative sleep. Our Naturopath Alison mixes up herbal formulas that are specifically formulated to address the reasons why you aren’t getting a good nights rest. There are many therapeutic herbs with clinical trials illustrating improvement in sleep quality and duration and a general feeling of wellbeing and quality of life. There are also specific nutrients in which studies have demonstrated anti-stress and sleep promoting properties. Alison discusses practices that you can introduce to help ensure you wake up refreshed and rejuvenated as well as giving you a Bowen treatment, that is sure to guarantee a great night sleep!
For more information on the vital role sleep plays on our health read the blog on our bio.
A good nights sleep can be a major determining factor in how we feel!
While we are sleeping our entire body repairs and regenerates mentally and physically. Sleep plays a vital role in memory consolidation and the release of hormones involved in the regulation of appetite and growth, which stimulates tissue repair, liver regeneration, muscle growth and the breakdown and conversion of fat to muscle. New research even shows that sleep may have a role in clearing neurotoxins implicated in the development of neurodegenerative diseases such as Alzheimer’s disease. (1)
As a nation, sleep deficiency is a major concern in Australia, with an estimated 20 -35% of the population experiencing disrupted sleep, inadequate sleep duration, daytime fatigue and excessive sleepiness.(2)
Acute and chronic sleep deficiency can also lead to physical and mental health problems. It can affect alertness, cognition, productivity, learning, mood and behaviour as well as being linked to many chronic health issues. Sleep deprivation can also dramatically weaken your immune system! (3)
Our body’s work on a circadian rhythm, or as we know it a “body clock”. When we wake up we expose ourselves to morning light and our body starts producing cortisol that makes us alert and energised. As the day progresses our cortisol levels reduce and as it gets dark we start to produce melatonin, the sleep or darkness hormone, which makes our body feel sleepy and restful. Many things can interrupt this circadian rhythm so sleep hygiene is a collection of practices around sleep that help promote melatonin production.
There are a number of herbal remedies and nutritional supplements that have been used in clinical studies that have been shown to have a profound effect on promoting good quality sleep.
- Xie L, Kang H, Xu Q, et al. Sleep drives metabolite clearance from the adult brain. Science 2013;342(6156):373-377.
- Mansfield DR, Hillman DR, Antic NA, et al. Sleep loss and sleep disorders. Med J Aust 2013;199(8):S5-6.
- Hart DR, The Brain Book. New Holland Publishers Pty Ltd. 2016
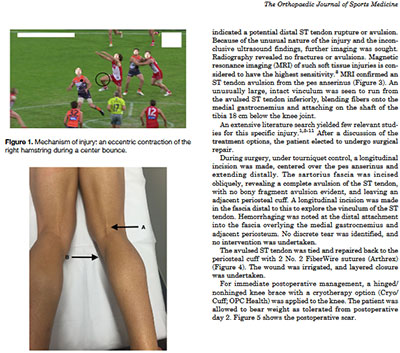
Distal Avulsion of the Semitendinosus Tendon
A Case Report
Hamstring injuries (including intramuscular injuries as well as proximal and distal hamstring tendon disruptive injuries) are some of the most common injuries in athletes.2 In Australian rules football, hamstring muscle injuries are the most common injuries suffered, with professional Australian Football League (AFL) clubs each sustaining an average of 6 injuries per season from their roster of 46 players.4 Hamstring injuries account for the most time lost from competitive sport (missed games) because of an injury in the AFL.7

Supporting Menopause Naturally
Menopause is a natural process where a woman transitions from her childbearing years to the next stage of her life.
At this time it's important for women to examine their stress levels, review their current lifestyle choices, and establish healthy habits. Hormones are one part of the picture in menopause, but they aren't the only contributor. Menopause has significant effects on a number of organ systems. Addressing all aspects of your body that influence your menopausal symptoms is vital when embarking on this next stage of life.
Whilst declining oestrogen is one of the reasons for hot flushes and night sweats, a common menopausal symptom, it is not the only cause. In fact, it is stress levels that play a larger role than oestrogen levels in triggering hot flushes. To highlight this, recent research has found that menopausal women have increased activity of the stress centre of the brain right before the onset of a hot flush.(1)
Therefore, it is vitally important to support a healthy stress response, not just hormones, to reduce menopausal symptoms.
Our Naturopath Alison can offer tailored support with this transition towards a balanced and energised mind and body. Specific herbs and nutrients can support healthy sleep patterns and nourish your stress response, and hence support your menopausal symptoms.
Physical menopausal symptoms
- Hot flushes
- Night sweats
- Aches and pains
- Bloating
- Crawling or itching skin
- Headaches/migraines
- Increased tiredness
- Sore breasts
- Urinary problems
- Vaginal dryness
- Wakefulness
- Weight gain
Emotional Menopausal symptoms
- Lowered mood
- Mood swings
- Feeling irritable
- Feeling anxious
- Reduced ability to cope
- Low libido
- Forgetfulness
- Reduced concentration
- Difficulty sleeping
- Increased PMS symptoms

Living Well With Osteoarthritis
Authored by Dr Adam Castricum
Sport and Exercise Physician
Osteoarthritis (OA) is a common condition affecting the joints of 11% of the Australian community. OA commonly follows injury to a joint and can occur years to decades after the initial injury, with increasing joint pain and stiffness with activity. In many however, OA can be associated with physical inactivity and obesity, with both conditions increasing the risk of many chronic diseases and with this premature disability and death. Currently there is no cure for OA. Fortunately, OA can be managed successfully for many years with a variety of non-surgical, exercise-based, load management interventions often without the need for more invasive surgery.
Sport and Exercise Physicians are specialist medical practitioners in the comprehensive non-surgical management of musculoskeletal problems, including osteoarthritis, often in the setting of chronic diseases such as diabetes, cardiovascular disease, cancer and mental illness. All Sport and Exercise Physicians at The Stadium Clinic have experience looking after elite athletes in team environments and apply these principles to the management of all patients, whether they are recreational athletes, manual workers, relatively inactive or those with or without chronic diseases simply wanting to safely manage their activity levels.
HOW SPORT AND EXERCISE PHYSICIANS CAN HELP YOU IF YOU HAVE OA
Sport and Exercise Physicians are specialist trained in:
- assessing and diagnosing musculoskeletal injuries including OA, and injuries that may lead to OA including shoulder dislocations, knee and ankle ligament injuries and hip and other smaller joint injuries
- devising and coordinating a comprehensive, multifaceted OA management program with an emphasis on safe return to activity and sport decisions as well as reducing the recurrence and severity of flares through appropriate load management strategies
- managing medical problems in the context of OA with exercise including
- asthma,
- obesity,
- heart disease,
- diabetes,
- cancer;
- mental illness;
- dementia
- prescribing exercise programs for the relatively inactive with OA and other chronic diseases
- assisting with the development and implementation of OA prevention programs at both a community and an elite sport level
Osteoarthritis is often a clinical diagnosis made on the basis of joint pain that is often worse with activity and may be associated with swelling, clicking, locking or instability and may be associated with a previous injury to the joint or surgery. The diagnosis is generally made on history and clinical examination, but can be confirmed with weight bearing x-rays. In certain circumstances, an MRI scan may be warranted. Ultrasound and CT scans should not be used to diagnose OA.
Initial management of osteoarthritis will in most instances be commenced by the General Practitioner or perhaps the allied health professional. For hip and knee OA, initial management should follow the guidelines in the recently released RACGP Guideline for the Management of Knee and Hip Osteoarthritis.
This should include
- education regarding OA, its natural time course and how it can affect your life
- reassurance that OA can be managed effectively with the correct treatment from a multi-disciplinary team
- advice, with the appropriate referrals regarding
- regular physical activity AND strengthening exercises
- where appropriate,
- weight loss through nutritional modifications and regular physical activity
- pain management if in the setting of chronic pain
- psychological support if associated mental health issues or illness
- appropriate judicious use of medications
Should you not improve with the above management, or require early specialist advice, a referral through your medical practitioner may be warranted to a specialist Sport and Exercise Physician for a more specific detailed consultation to help you manage and live better with OA.
Following a thorough history, clinical examination and review of any imaging with a Sport and Exercise Physician, the appropriate treatment plan for your OA can be developed with your life and activity goals in mind. This involves comprehensive advice on activity and exercise that can be safely undertaken, the appropriate rehabilitation program, possible interventions including the appropriate joint injections and return to activity decisions. Sport and Exercise Physicians are experts in the appropriate load management for joints with OA and will be able to prescribe an individualised joint strength and activity program which can help you get back to the activities you enjoy. This may be in the form of brisk walking, cycling, swimming, gardening, hiking, climbing, ball sports, snow sports, pilates, gym, yoga and even running, yes running. These activities, appropriately prescribed, may also help slow the progression of OA, preventing the need for surgery. Even better, regular physical activity will help prevent and indeed improve any other chronic diseases you may have.
Where further specialist allied health and other medical specialist advice is warranted, rapid referral to the appropriate practitioners can be arranged. The multi-disciplinary allied health team can include sport and exercise / musculoskeletal physiotherapists, exercise physiologists, osteopaths, chiropractors, podiatrists, sports dietitians, myotherapists, and psychologists. Sport and Exercise Physicians work closely with Orthopaedic Surgeons and understand when surgical intervention is required and can facilitate timely referrals to help get patients moving again, when all non-surgical treatments have been exhausted.
GP’s can assist patients with timely facilitation of referrals onto sports psychologists, physiotherapists, exercise physiologists and other members of the allied health team to access the Medicare rebate for these services in the setting of mental health or Team Care plans respectively.
FAQS
Do I need a referral?
A medical referral is required to see a Sport and Exercise Physician, if you wish to claim the Medicare rebate for the consultation. GP referrals are valid for 12 months from the initial consult. Other medical specialist referrals are valid for 3 months from the initial consult.
A medical referral is not required to see a Sport and Exercise Medicine Registrar. All ACSEP Registrars at OPSMC are supervised by Sport and Exercise Physicians are all accredited trainees of the Australasian College of Sport and Exercise Physicians (ACSEP). They have completed the pre-requisite medical and hospital-based training.
What do I need to bring to the consultation?
You are asked to please bring:
- Your GP / specialist referral and any other treating practitioner referral
- ALL previous imaging (films, discs and reports) relevant to the presenting condition.
- Pathology results and other special investigations
- Comfortable clothes to change into for the examination part of the consultation.
How long do consultations take?
Initial consultations are generally up to 40 minutes in duration. Review consultations can take up to 20 minutes, but these are at the discretion of the Sport and Exercise Physician / Registrar
Can I get a rebate?
All consultations are Medicare rebateable provided you have a valid GP or specialist medical referral. It is up to you to ensure your current referral is up to date. The Medicare rebate for the initial and review consult are similar to that for Specialist surgeons and are not time based. You may also eligible for a Medicare rebate for an ultrasound guided injection provided it complies with the Medicare guidelines and you have a valid referral.
Consultations with Sport and Exercise Medicine Registrars attract nonVR-GP Medicare rebates, at a significantly lower rate than specialist Sport and Exercise Physicians. These consultations are time based.
Consultations with Sport and Exercise Physicians are not eligible for rebates through Private Health Insurance schemes.
For full details of consultation fees, please refer to the Practitioner fee statement on the online booking site or contact the clinic.
Can a Sports and Exercise Physician refer me for a rebateable MRI Scan?
As Specialists, Sport and Exercise Physicians can refer for rebateable MRI scans, on most body parts, provided they adhere to the Medicare Benefit rules. Sport and Exercise Medicine Registrars, like GP’s, can refer for limited GP rebateable MRI scans again provided they adhere to specific Medicare guidelines.
Further information can be found through the Australian Commission on Safety and Quality in Health Care Osteoarthritis of the Knee Clinical Care Standard fact sheet and this Decision Tool for patients

Safe and Natural Support for Pregnant Women in the cold and flu season
Expectant mothers are often prone, more so than usual, to colds and flus, coughs and sore throats especially as the winter season progresses. Good rest, a healthy balanced diet and plenty of water is of course important for a quick recovery, however there are some other useful safe natural remedies that can help reduce the uncomfortable cold and flu symptoms whilst also helping your immune system to fight off viruses faster and more effectively.
At the first sign of a cold, if you have been exposed to someone who has a cold it may be helpful to take Echinacea purpurea, a herb that has been used for centuries in Western herbal medicine.1 It is used in acute and chronic viral and bacterial `\respiratory conditions including the common cold, sinusitis, ear infections and bronchitis. Echinacea is a category A medicine in pregnancy, indicating that controlled studies in healthy pregnant women demonstrated no foetal risk 2. So Echinacea can be safely taken during pregnancy.
Other nutrients that are essential in the maintenance of a healthy immune system during pregnancy are zinc and vitamin C.3 When taken within 24 hours of the first symptoms of infection, zinc reduces the severity and duration of colds by boosting the production and function of WBCs.4 ,5 Similarly vitamin C reduces symptom severity and duration of the common cold by an average of 23%.6
Great sources of vitamin C in winter include potatoes, broccoli, parsley, thyme, peppers, brussel sprouts, savoy and red cabbage, cauliflower, dark green leafy vegetables such as kale, citrus fruits such as mandarins and oranges, kiwifruit and strawberries.
Frozen vegetables and fruit picked at their season best and frozen immediately before nutrients like vitamin C have deteriorated are great healthy and convenient choices during the winter months. For example frozen spinach can be thrown into a pasta sauce, casserole or soup to add extra nutrition. Likewise peas can be added to many meals such as brown rice and quinoa with herbs and spices. Frozen berries are a fantastic source of vitamin C and can be used in smoothies, a crumble or added to yoghurt and muesli for a wholesome breakfast.
Food high in zinc include organic grass fed meat, poultry, fish, legumes including beans, lentils and chickpeas (best soaked overnight for better absorption). Seeds are a great source of zinc including hemp, chia, sunflower and pumpkin seeds. Nuts are an easy way to get zinc as well as many other minerals and are a nutritious snack particularly peanuts, cashews, almonds and pine nuts or alternatively try a nut butter. Other sources of zinc are whole grains, eggs and dairy such as cheese and milk. In general, zinc absorption from a diet high in animal protein will be greater than from a diet rich in plant derived proteins.3
Getting enough rest and sleep is essential for a quick recovery from colds and flus. Traditional remedies such as chicken soup, lemon grass and ginger tea with a teaspoon of honey, consumption of plenty of garlic and fresh vegetables and steam inhalations to help clear blocked sinus all help with the uncomfortable symptoms of a cold.
It is important to speak to your healthcare practitioner for more information about supplementation that is specifically indicated for you at this precious time.
References
- Mills S, Bone K. The essential guide to herbal safety. Elsevier Health Sciences, 2005
- Echinacea purpureamonograph. Health Canada. Viewed 17 May 2017, http://webprod.hc-sc.gc.ca/
- NHMRC. Nutrient reference values 2006. Viewed 7 August2019, https://www.nrv.gov.au/
- Singh M, Das RR. Zinc for the common cold. Cochrane Database Syst Rev. 2011 Feb 16;(2):CD001364. doi: 10.1002/14651858.CD001364.pub3.
- Barnett JB, Dao MC, Hamer DH, Kandel R, Brandeis G, Wu D, et al. Effect of zinc supplementation on serum zinc concentration and T cell proliferation in nursing home elderly: a randomized, double-blind, placebo-controlled trial. The Am J Clin Nutr. 2016 Jan 27;103(3):942-51. doi: 10.3945/ajcn.115.115188.
- Hemilä H. Does vitamin C alleviate the symptoms of the common cold?-a review of current evidence. Scan J Infect Dis. 1994 Jan 1;26(1):1-6. PMID: 8191227.

Coffee with Cynthia: Dr Tom Cross
Sydney Swans No. 1 ticket holder Cynthia Banham is an accomplished journalist and author. In a series for sydneyswans.com.au she has spoken with club staff to delve deeper into what makes the team behind the team tick. This week she's caught up with Sydney Swans club doctor, Dr Tom Cross.

Tips from our Naturopath on keeping well this winter
Winter can be a trying time both mentally and physically, the days are shorter, colder and darker and our bodies become susceptible to colds and flus. One way to avoid becoming run down and consequently sick is to slow down! Winter hibernation is the ideal time of the year for our bodies to heal and rest.
Try to avoid rushing. Instead make a concerted effort to embrace a slower more relaxed pace during the cold winter months. Balance out your social engagements with some quiet time at home like reading a book or making time for meaningful relationships with family and friends.
Good sleeping habits, ideally rising at 7am and retiring at 10pm at the latest will help with our vitality and strengthen our bodies in the winter months.
Another way to support optimal health through the winter months and change how you are feeling whether physically or emotionally is to exercise. If you are feeling overextended and tired, opt for gentle exercises like walking, Tai Chi or Yoga. If you are feeling sluggish and heavy, go for a more vigorous workout like a bike ride, a jog or a gym session.
As soon as you get any signs of coming down with a cold or flu …stop and slow down!
For further information about Alison Gallagher visit our website www.stadiumclinic.com.au

Holistically Supporting Adolescents in times of Stress
No one will dispute the fact that the teen years can be a challenging time with the pressure of school work, sport, friends, family, part time jobs plus the pressure and constancy of social media. This alone is enough to cause considerable stress however when teens are presented with a health concern or sports injury, additional strain is added to an already demanding time.
The 2018 Stress in America survey of adults and teenagers found that high school students have higher stress levels than adults. 1
Our lifestyles are very different to how our ancestors lived yet our bodies and brains are exactly the same. Our ancestors lived in close knit communities, socialised together, told stories, drew on cave walls, walked in the forest for most of the day hunting or gathering food, had spiritual rituals, lived close to nature, ate clean healthy diets and slept when it was dark.
Compare this to how our kids and teenagers live today. Firstly they go to sleep later, often lying in bed on their iphones or laptops, exposed to blue light. Such Exposure to this light at night interferes with your circadian rhythm and suppresses melatonin secretion. Melatonin is made in the pineal gland and is the hormone that controls our sleep and wake cycles.
In the morning children rush to school often with no breakfast or a sugary processed cereal at best. They are under academic pressure at school, have hours of homework and often lots of after school activities. If you add any other additional stresses that are prevalent in our society, you have a very stressed young person.
When you experience anxiety your stress hormones, adrenaline and cortisol, increase and can cause a ‘fight or flight' reaction which turns on our sympathetic nervous system (SNS). This reaction gets the body ready to run away or fight danger. Our heart rate, blood pressure and blood sugar levels increase and blood flows to our big muscles needed to deal with whatever threat has presented itself.
We rarely need to escape from life threatening situations in our Western society as many of our anxiety provoking situations are more in our minds. Therefore as we are not using our physical body to sprint from danger and so our stress hormones are not lowered. If we keep experiencing stress these hormones build up and can create chronic health problems over time. Hence the reason why exercise is essential for reducing stress levels.
Some of the symptoms of stress include shaking and trembling, sweaty palms, a racing heart, difficulty breathing and dizziness. In the long term if the body is in a state of chronic stress less energy is available for other body systems to function optimally. For example digestion, and immune system functions are compromised, which is seen in many children and teenagers suffering from chronic digestive problems such as irritable bowel or chronic infections such as glandular fever.
For a holistic approach to support young adults it is essential to address diet, nutritional deficiencies, exercise, lifestyle and sleep.
As a Naturopath I include nutrition, herbal medicine, homeopathy, Bach flower essences and Bowen therapy as an ideal treatment option for teenagers. With a focus on prevention and individualised treatments I am able to listen to and understand the unique experiences and symptoms for each teen and tailor a treatment plan to their needs.
References
1. Viktorinova A, Ursinyova M, Trebaticska J, et al. Changed plasma levels of zinc and copper ti zinc ratio and there possible associations with parent- and teacher rated symptoms in children with attention-deficit hyperactivty.

Improving sleep with Bowen therapy
Australian surveys have shown upto 33 per cent of the adult population have difficulty getting to sleep or staying asleep. A recent Federal government inquiry called for sleep to be made a national priority and recognised it as a third pillar of a healthy lifestyle along with diet and exercise.
Symptoms of insomnia, such as mind chatter, worry, stress and increased activation of the sympathetic nervous system overlap considerably with anxiety and depression.
Bowen therapy is a gentle form of body work that has a calming effect on the nervous system and relaxing tight muscles. Bowen therapy works by lowering the stress response and bringing a sense of balance and grounding to the body. Using Bowen therapy, a shift occurs whereby the body moves from the sympathetic nervous system to the parasympathetic nervous system, (which is known as the "rest and digest system") thereby being responsible for bringing the body back into equilibrium after activation of a stress response.
Bowen has the benefit of working immediately to reduce stress levels and improve the quality of sleep.

Franklin Does the Honours for Clinic
Star Sydney Swans forward Lance Franklin this week opened the club's official doctor's clinic in the heart of Moore Park. The Stadium Clinic has played a central role in getting Sydney's players on the ground week in and week out since being founded at Moore Park in 2008, but the rebuild of Allianz Stadium has seen the practice relocate to the Byron Kennedy Hall in the Entertainment Quarter.

Research Publication Co-Authored by Dr Tom
Cross
The Franklin-Naismith Lesion
A Severe Variant of Hip Pointer
This case report presents 2 professional Australian rules football players from the Sydney Swans Football Club who sustained a serious variant of the hip pointer injury during match play.
Dr Tom Cross and Sinem Gultekin outlines the clinical presentation, investigation, and management of this rare but important injury.

The Stadium Sports Medicine Clinic isn't your average facility. It's the place that looks after some of Australia's biggest sporting stars including Buddy Franklin and Israel Folau.